Jack Willard ’24: Boston Medical Center
- The Rivers School

- Sep 8, 2023
- 4 min read
You may not often stop to think about how important your hands are in carrying out even the most mundane daily tasks. That is, until something goes wrong with them, and if there’s anything I’ve learned from my seven-week internship in the Orthopaedic Surgery Department at Boston Medical Center, it’s that there’s a lot that can go wrong with your hands. This summer, I had the incredible opportunity to work with hand and upper extremity surgeon Dr. Andrew Stein and observe dozens of surgeries in the operating room as well as hundreds of appointments in the outpatient clinic. What made my experience most unique was working with patients from all racial, cultural, linguistic, and socio-economic backgrounds due to BMC’s status as a safety net hospital, meaning care is given to patients regardless of their ability to afford it. I couldn’t be more grateful to have learned so much about orthopaedics, patient care, and the many people that make BMC a world-renowned academic medical center.
I began my internship by observing the department’s daily board rounds on Zoom at 5:15 a.m., where the orthopaedic surgery residents discussed cases that had come into the Emergency Department that night. These cases could range from joint pain to infections to stab and gunshot wounds. In these meetings, every case was reviewed thoroughly, and the attending surgeons used each one as a teaching opportunity to enrich the residents’ training. After a week of observing rounds, I came to BMC in person to shadow Dr. Stein, Dr. Alley (a senior resident), and several physician assistants in the clinic and operating room. During the two days a week that the surgeons saw patients in the clinic, they went between appointments nonstop for up to eight hours, so I appreciated that they still found time to tell me about each patient’s diagnosis, x-rays, or treatment plan. Common conditions that patients presented with included carpal and cubital tunnel syndrome, trigger finger, medial and lateral epicondylitis (also known as “tennis” or “golfer’s” elbow), and arthritis. It was interesting to learn the anatomy behind conditions that I had only heard of before, as well as more serious conditions such as tendon ruptures, nerve lacerations, and wrist fractures. Occasionally I would shadow orthopaedic surgeons that specialize in joints, spine, and sports medicine as well. I was also pleased to be able to help the providers communicate with Spanish-speaking patients and observe the vital work done by medical interpreters.
X-Rays of a metacarpal fracture, stabilized with screws Dr. Stein repairing a ruptured tendon in the OR
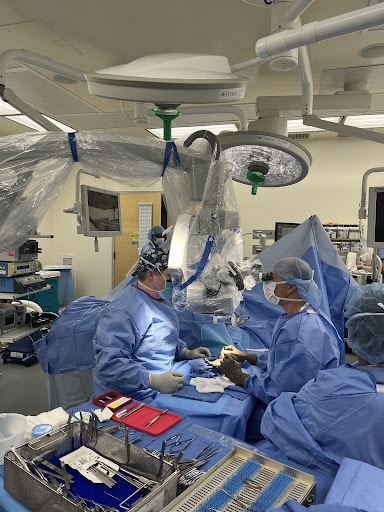
On Tuesdays and Thursdays, I was with Dr. Stein and Dr. Alley in the operating room. On my first day, I watched the surgeons repair the ruptured tendon and lacerated nerve of two stabbing victims. In another procedure, Dr. Stein extracted stem cells from a patient’s hip bone to repair a fracture in the distal radius below the wrist. I learned how the surgeons scrubbed and put on a sterile gown before every procedure and how the nurses prepped the patient for surgery. Every member of the OR team, including the nurse, scrub tech, and anesthesthetist, had a vital role to play in making sure each procedure went smoothly. I was also able to observe several other procedures outside of hand surgery, including hip and knee replacements, a prostectomy, and several shoulder, spine, trauma, and sports medicine cases.
Wearing a mask, bouffant cap, and eye wear in the OR Dr. Stein repairing a lacerated nerve with a microscope
On Friday mornings, I accompanied the residents to what they called “bone school,” a weekly lecture given by an attending surgeon as part of their residency curriculum. After the lecture, they would review the topic discussed by doing practice questions that could appear on their yearly exams. The attendings and senior residents also organized interactive activities for the interns (first-year residents) such as an augmented reality surgery presentation and a workshop on applying casts. After bone school, I shadowed Dr. Wang, a second-year resident, as she did orthopaedics consults in the Emergency Department and in-patient wards. She was responsible for answering pages from all other departments that required assistance from an orthopedist, so she was extremely busy seeing patients or dictating patient notes for the rest of the day. However, even she managed to answer questions I had about a patient or their condition, which I greatly appreciated.
Set up for the AR surgery presentation Residents putting a splint on me during a workshop
The final part of my internship that I am still working on is writing a surgical case study with the help of Dr. Stein and Dr. Kim, a fourth-year resident interested in pursuing hand surgery as a subspecialty. In the case study, we discuss a patient who had a tear in the volar scapholunate ligament of their hand. Dr. Stein successfully reconstructed the ligament in the operating room, and a surgery of this type had not been done before, so I’m grateful for the opportunity to help document the case, which can hopefully get published to contribute more knowledge to the field. I’m amazed that I get to collaborate with two incredible surgeons and take part in this kind of medical research as a high school student.

Working with Dr. Stein and the Orthopaedic Surgery Department at BMC has been the best summer experience I could have asked for. I’d like to give a huge thank you to Dr. Stein and all of the BMC staff that I got to meet for being so welcoming, patient, and kind over my seven weeks. A special thank you to Drs. Maxwell Alley, Carol Wang, and Eugene Kim for your support. And finally, a big thank you to Mr. Schlenker and the Rivers School science internship program for this opportunity.


















Comments